Why Steroid Is Not the Only Injection Option in Musculoskeletal Medicine
Understanding Injection Options for Knee Osteoarthritis
If you are struggling with knee pain from osteoarthritis, you may have been told that a steroid injection could help. However, it is important to understand two things:
- What any injection can realistically achieve.
- That steroid is not the only option available.
As a Consultant in Sports and Exercise Medicine, I believe patients should understand the full range of evidence-based options so they can make informed decisions about their care.
What Can Injections Actually Do in Knee Arthritis?
This is usually the first and most important question. Patients often ask whether an injection will “repair the damage” inside the joint. The key point is this: no injection reverses arthritis.
The aim of any injection in knee osteoarthritis is to improve the environment within the joint — reducing pain and stiffness to create a window of opportunity. That window allows you to rebuild strength, restore movement and improve function.
Realistic expectations are critical. An injection will not turn back the clock on your knee. But months or years of pain reduce strength, limit activity and negatively affect overall health — all of which can make arthritis feel worse. Trying to reverse those changes while every step is painful is extremely difficult.
The best outcomes occur when an injection is used strategically — to create short-term symptom relief that enables medium- to long-term rehabilitation.
What Do Steroid Injections Actually Do?
Corticosteroid injections reduce inflammation within the joint. In knee osteoarthritis, they can be particularly helpful during an acute flare when the joint is swollen and irritated.
They can:
- Reduce inflammation.
- Improve pain in the short term.
- Act quickly.
- Create a window for rehabilitation.
However, they do not regrow cartilage, reverse osteoarthritis, or repair structural joint changes. For most patients, the benefit lasts weeks to a few months.
Steroids are powerful anti-inflammatory medications, but there is evidence that repeated use within the same joint may have a negative impact on cartilage. In some cases, frequent injections may accelerate degenerative change. This is why repeated steroid injections are rarely a long-term strategy. This does not mean steroid injections should not be used; it means they must be used thoughtfully and selectively.
Other Injection Options Patients Should Know About
Steroid is not the only injectable treatment available. Depending on the stage of arthritis, age, activity levels and goals, alternative options may be more appropriate. These can be particularly relevant for younger or more active individuals who wish to minimise potential cartilage effects and maintain long-term joint health.
Hyaluronic Acid
This treatment provides lubrication and shock absorption. It is best suited for people with mild to moderate arthritis.
Platelet-Rich Plasma (PRP)
This uses concentrated parts of your own blood to balance the environment inside the joint. It is best for early-stage arthritis and active individuals.
Corticosteroids
These are used for the rapid reduction of swelling and inflammation. They are best for sudden pain flares and short-term relief.
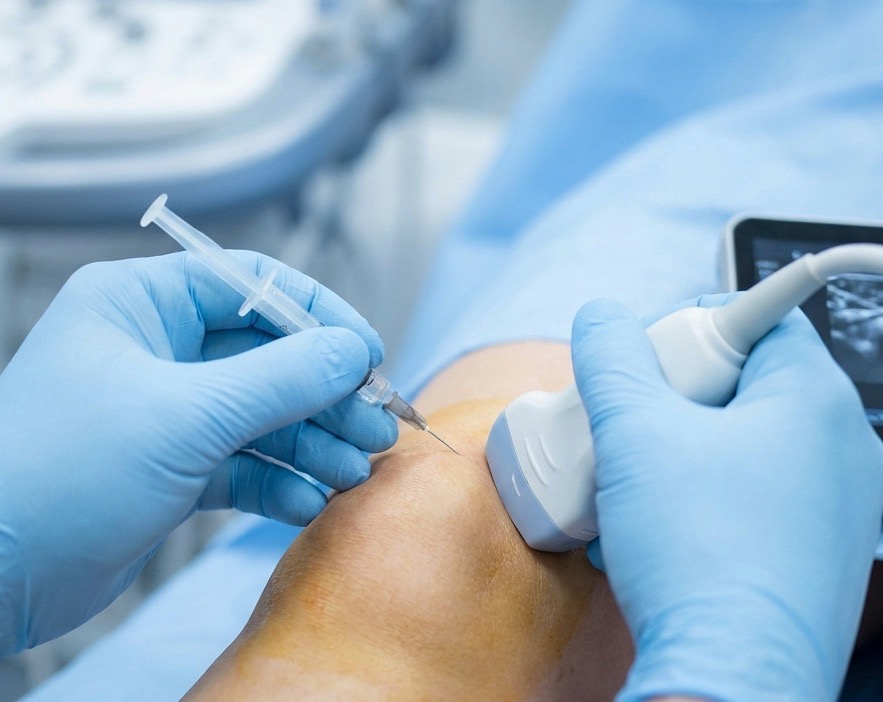
Image-Guided Precision Injections
Ultrasound guidance improves accuracy, ensuring the medication is delivered precisely into the joint or targeted structure. Accuracy matters, particularly in more complex cases. Not every injection is suitable for every patient. The right choice depends on clinical assessment, imaging findings, symptoms and long-term goals.
Osteoarthritis Is More Than “Wear and Tear”
Osteoarthritis is not simply cartilage thinning. Pain is influenced by various factors:
- Inflammation.
- Muscle weakness.
- Joint loading patterns.
- Nervous system sensitivity.
- Sleep, stress and general health.
This explains why scan findings do not always match pain levels. It also explains why no injection, on its own, is ever the full answer.
Exercise Remains the Foundation
While injections can reduce pain, the strongest long-term evidence in knee osteoarthritis supports structured exercise. Targeted strengthening improves joint stability, shock absorption, load distribution and confidence in movement.
Exercise builds resilience within the joint. When injections are used appropriately — whether steroid, hyaluronic acid or PRP — they should complement rehabilitation, not replace it.
A Comprehensive, Individualised Approach
Two patients with the same X-ray findings may require completely different strategies. A proper assessment helps determine if inflammation is the primary driver, if weakness is the main contributor, or which injection is most appropriate for an active individual.
The goal is not simply to reduce pain today; it is to improve long-term function and joint health. In musculoskeletal medicine, the best results come from combining the right intervention with the right rehabilitation — tailored to the individual.
The Take-Home Message
Steroid injections are one option, but they are not the only one. There are different indications, and there should always be a plan beyond the injection itself. If you are considering an injection for knee arthritis, the most important first step is not choosing the injection — it is having the right assessment.
Understanding which treatment is appropriate for you, at your stage of arthritis, with your goals and activity levels, makes all the difference.
Because successful treatment is not about finding a quick fix.
It is about choosing the right strategy.